Demystifying Obstructive Sleep Apnea (OSA)
What is Obstructive Sleep Apnea?
Obstructive Sleep Apnea (OSA) is a chronic, serious, and most common sleep disorder. It occurs when the throat muscles relax during sleep, causing complete or almost complete airways collapse, cutting off airflow intermittently. Many people think of sleep apnea as just loud snoring; however, sleep apnea when untreated can lead to significant morbidity and mortality. Although all the muscles in the body relax when we sleep, people with naturally narrow throats or large neck size are more prone to sleep apnea. When the airflow gets cut off, oxygen levels go down, and your brain kicks in a survival reflex that momentarily wakes you up so you can breathe again. This reflex is vital for staying alive, but it messes up your sleep, leaving you feeling tired.
Recognizing the Symptoms
People with sleep apnea could suffer from symptoms during the night as well as during the day. These can vary from person to person. Many people don’t realize that they have sleep apnea until a partner, family member, or roommate notices something unusual during their sleep and/or during daytime.
Nighttime Symptoms
- Loud Snoring: This is the most common symptom, occurring when air pushes through a narrowed airway. However, not everyone who snores has sleep apnea, and not everyone with sleep apnea snores.
- Breathing Pauses: If you share a bed, your partner might notice you stop breathing temporarily while sleeping. This is scary and concerning for bedpartners.
- Gasping or Choking: When your throat closes during sleep apnea, this may cause you to wake up feeling short of breath or as if someone is trying to smother you. You might feel like you need to catch your breath.
- Restless Sleep: Sleep apnea often leads to frequent awakenings and difficulty staying asleep, also known as sleep maintenance insomnia.
- Frequent Urination at Night: Waking up multiple times during the night to urinate is a common symptom that many individuals overlook.

Daytime Symptoms
- Dry Mouth & Morning Headaches: Many people with sleep apnea wake up with a dry mouth, sore throat, drooling, or even headaches, all because of not sleeping well and not getting enough oxygen at night. They can be mouth-breathers.
- Non-restrorative Sleep: Despite getting adequate amounts of sleep, people with sleep apnea tend to wake up feeling as if they have not slept enough. They feel tired in the morning.
- Excessive Daytime Sleepiness: It is also known as hypersomnia. It can be so severe that you may feel sleepy even when you are driving, listening to lectures, watching TV or even talking to someone.
- Brain fog and Cognitive Issues: Sleep apnea disrupts the brain’s oxygen supply, and this lack of adequate oxygen can negatively affect attention, concentration, and memory retention.
- Mood Changes: Not getting enough sleep over time can make people feel cranky, anxious, or even depressed. Some patients with sleep apnea tend to snap easily at others.
Causes and Risk Factors
OSA is caused by a combination of lifestyle, anatomical, biological, genetic, and positional factors.
- Lifestyle: Certain factors like obesity and alcohol are linked to OSA. Obesity is the most common cause of OSA in adults. Extra fat around the neck increases soft tissue in the throat, which can block the airway. Even a 10% increase in body weight can raise the risk of OSA by sixfold. Also, drinking alcohol six hours before bedtime can relax your throat muscles too much, making it easier for your airway to collapse.
- Anatomical: Structural features like narrow throat, large tonsils, recessed or small jaw, a thick neck (over 17 inches for men, 15 inches for women), or a deviated nasal septum increase risk of OSA.
- Biological: Age and gender play an important role in OSA. It tends to be more common in older adults (50 or above) and is 2-3 times more common in men than women. Notably, the risk of OSA is higher in post-menopausal women.
- Genetics: A family history of OSA or if someone has genetic conditions (Prader-Willi Syndrome (PWS), acromegaly, etc. have been strongly linked to OSA.
- Medications: Certain medications cause significant relaxation of airway muscle resulting in airway collapse leading to an increased risk of OSA. These medications include sleeping pills, narcotics, muscle relaxants, and anxiolytics.
- Positional: Sleeping on back raises the risk of OSA by allowing the tongue and soft throat tissues to narrow or block the airway.
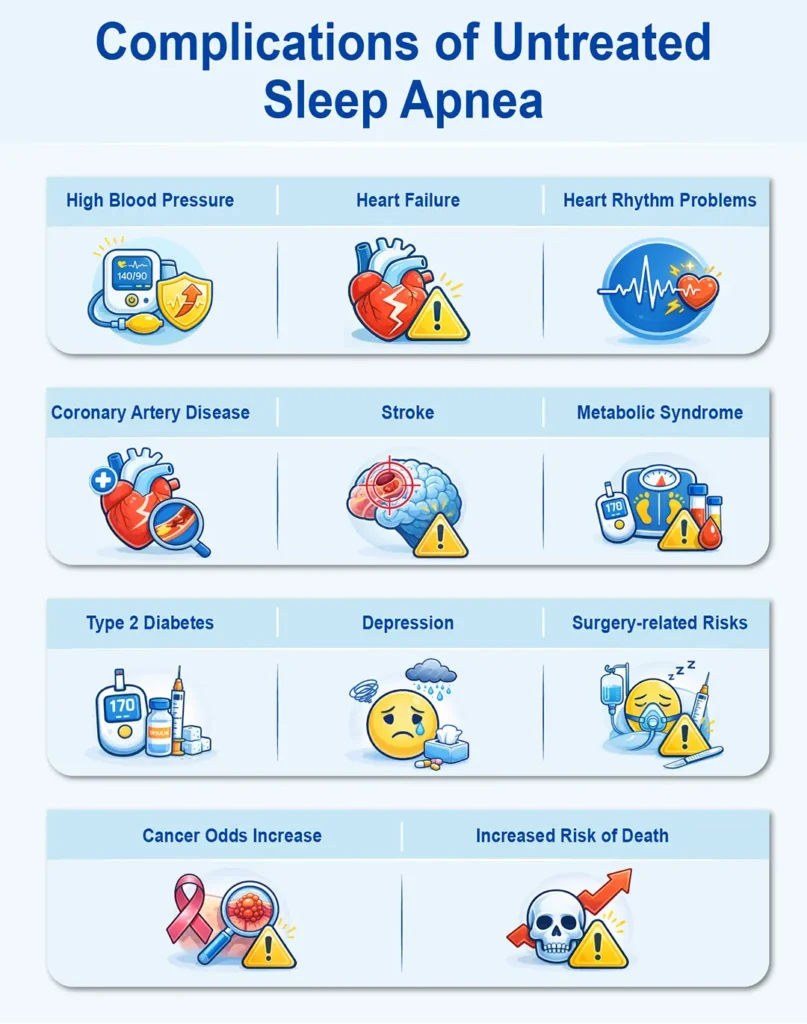
Consequences of Untreated Obstructive Sleep Apnea
Obstructive Sleep Apnea is not just a sleep problem, it is a whole-body disease that affects multiple organs. If left untreated, the consequences can be life-threatening.
Cardiovascular Health
Sleep apnea places immense stress on the heart. It is a strong, independent risk factor for high blood pressure; about 50% of sleep apnea patients suffer from high blood pressure. The repeated drops in oxygen strain the cardiovascular system, increasing the risk of heart failure, coronary artery disease, and stroke. Furthermore, abnormal heart rhythms, particularly atrial fibrillation, are very common in patients with sleep apnea.
Brain Health
Poor oxygen supply during sleep can damage the brain over time. Sleep apnea has been linked to memory loss, difficulty concentrating, and a short attention span. It has been associated with neurological diseases such as Alzheimer’s dementia and Parkinson’s disease.

Metabolic Health
Sleep apnea has been linked to metabolic syndrome and type 2 diabetes. Sleep apnea negatively affects how the body handles sugar, leading to poor glucose metabolism and insulin resistance.
Mental Health
People with untreated sleep apnea often experience mood swings, irritability, anxiety, and depression. Ongoing poor sleep can also reduce focus, motivation, and overall quality of life.
Surgical Risks
Untreated sleep apnea increases the risk of serious complications during surgeries especially those where general anesthesia is used. These surgical risks include respiratory failure and cardiac arrest.
Cancer Risk
Research suggests a troubling link between sleep apnea and certain cancers. Low oxygen levels during sleep may encourage tumor growth and worsen cancer outcomes.
Motor Vehicle Accidents
Studies have shown that OSA patients tend to get into fatal head-on MVA collisions more while driving. Sleepy drivers tend to have more lane drift.
Diagnosis of Sleep Apnea
Diagnosing sleep apnea begins with a medical evaluation of your sleep habits, symptoms, and risk factors. If your clinician suspects sleep apnea, they will recommend a sleep test to look for it.
Types of Sleep Studies Used for OSA Diagnosis
Below are some types of sleep studies used to diagnose sleep apnea and observe the activity of your brain, heart, lungs, and body during sleep.
Polysomnography (In-Lab PSG)
This is considered the gold standard and most comprehensive sleep study for diagnosis of sleep apnea. Conducted in a sleep center where patients are video and audio recorded. This study is used to monitor the following during sleep: Brain activity, sleep stages, sleep time, eye movements, heart rate and rhythm, breathing effort, oxygen level, snoring, body position, leg movements and abnormal sleep behavior. It can identify other disorders in addition to sleep apnea like periodic limb movements, insomnia, parasomnias, etc.
Cons: Inconvenient, long wait time and expensive.
Home Sleep Apnea Test (HSAT)
A home sleep apnea test is a simplified version that is designed to only look for sleep apnea, hence, the name, Home Sleep Apnea Test. While convenient, affordable, comfortable and is able to detect most cases of moderate-severe OSA, HSAT is less detailed than in-lab studies and cannot diagnose other disorders. It tends to miss sleep apnea in 10-15% of cases, therefore, when negative, further evaluation with PSG is recommended. There are different types of home sleep apnea tests available in the market. They can be disposable or reusable. They can be single or multiple nights.
Home PSG (Polysomnography)
A home PSG is a newer-type of comprehensive home sleep study. It is comparable to traditional in-lab PSG. It is designed to detect other sleep disorders in addition to sleep apnea. It monitors brain activity, sleep stages, sleep time, eye movements, heart rate and rhythm, breathing effort, oxygen level, snoring, body position and leg movements. For patient’s own privacy, there is no video recording during Home PSG.
Top 6 Reasons to Get a Sleep Study
Getting a good night’s sleep isn’t always easy. Despite going to bed on time, someone might wake up feeling tired or groggy. Sleep studies help doctors understand what’s happening while you sleep and find ways to improve it.
Here are six ways a sleep study can help you:
- Find the Problem: Sleep studies track sleep patterns, breathing and oxygen levels during sleep. This helps detect issues like pauses in breathing that may otherwise go unnoticed. Sleep studies can help diagnose sleep disorders like sleep apnea, insomnia, etc. Knowing the exact issue is the first step toward getting better sleep.
- Personalized Treatment: Doctors can use the results to create a customized-treatment plan. This ensures that the solution addresses the patient’s unique sleep challenges.
- Feel More Alert During the Day: Treating sleep problems can make a huge difference how people feel during the day. Better sleep improves focus, memory, and overall energy levels.
- Protect Your Health: Untreated sleep problems can increase the risk of heart disease, high blood pressure, diabetes, mental health and other health issues. A sleep study can help prevent these long-term risks.
- See if Treatment Works: A sleep study can help decide if treatment for sleep apnea is working or not. It may also help to adjust therapy.
- Guide Lifestyle Changes: Doctors can use the results to suggest helpful changes in your habits, diet, or bedroom environment. Even small adjustments can lead to big improvements in sleep quality.
In short, a sleep study is about better understanding your sleep and making sure your body and mind get the rest they need. After all, good sleep is the foundation of a healthy, happy life!
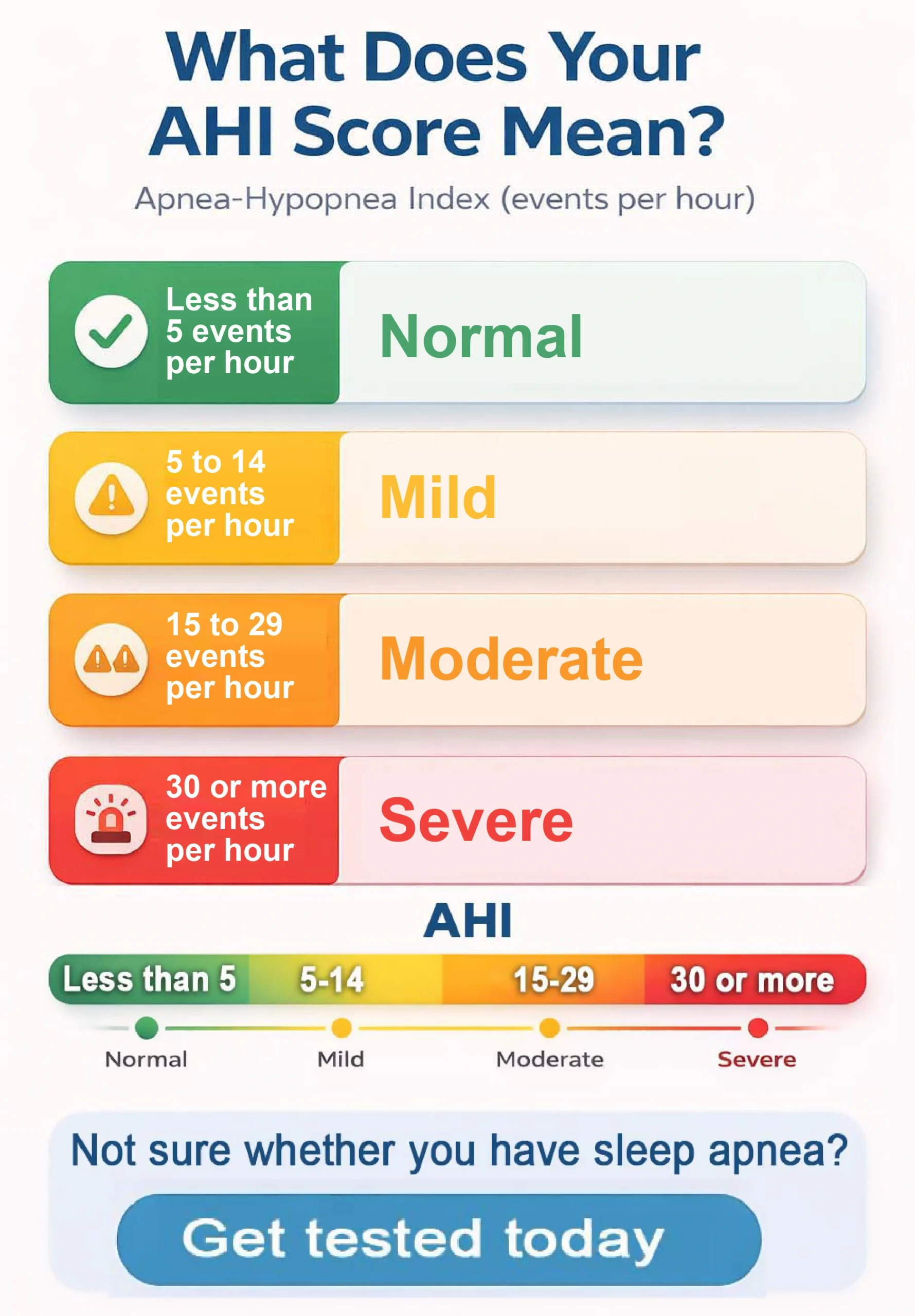
Severity of OSA
The severity of OSA is usually determined by Apnea-Hypopnea Index (AHI) which is a sum of apnea and hypopnea events per hour. An apnea event is when you stop breathing completely for at least 10 seconds due to complete collapse of the airway leading to absence of airflow. While a hypopnea event is caused by partial collapse of airways causing reduced airflow and oxygen drop by 3-4%.
Treatment Options
Treatment of sleep apnea is not one size fits all, it needs to be tailored-based on the severity of sleep apnea and patient preference.
Let’s take a look at some of the treatment options for OSA.
Positive Airway Pressure (PAP) Therapy
If diagnosed, the most common and effective treatment is Positive Airway Pressure (PAP) therapy. These devices deliver pressurized air through a hose and mask to keep the upper airway open during sleep. Success with PAP therapy requires good compliance, regularly cleaning the equipment and working with their clinician to resolve issues. Following all these steps optimizes the chances of successful treatment. Some types of these devices include:
 CPAP (Continuous Positive Airway Pressure) Therapy: The most well-studied device for the treatment of sleep apnea is CPAP. It provides a steady stream of the same positive airway pressure during inspiration and expiration. It splints open the airway during sleep and prevents it from collapsing. This leads to optimal oxygen supply to the vital organs of the body during sleep, improves sleep quality and minimizes the risk of serious complications of untreated sleep apnea like heart attacks and stroke.
CPAP (Continuous Positive Airway Pressure) Therapy: The most well-studied device for the treatment of sleep apnea is CPAP. It provides a steady stream of the same positive airway pressure during inspiration and expiration. It splints open the airway during sleep and prevents it from collapsing. This leads to optimal oxygen supply to the vital organs of the body during sleep, improves sleep quality and minimizes the risk of serious complications of untreated sleep apnea like heart attacks and stroke.- APAP (Auto-Adjusting PAP): These machines automatically adjust air pressure based on your breathing patterns and snoring throughout the night.
- BiPAP (Bilevel PAP): Designed for those who struggle with standard CPAP, BiPAP provides higher pressure when inhaling and lower pressure when exhaling, making it easier to breathe out.
Oral Appliance Therapy
These are also known as Mandibular Advancement Devices (MADs). For patients with mild to moderate sleep apnea who cannot tolerate CPAP, oral appliances are a valuable alternative. These are custom-fitted titratable devices which cover the upper and lower jaw and gently pull the lower jaw forward. This in turn creates space in the back of the throat and opens the airway. It is crucial that these devices are custom-fitted by a dentist trained in sleep medicine to ensure effectiveness and monitor for side effects like bite changes.
eXcite OSA
This is a relatively newer technology used during daytime to treat snoring or mild OSA. It works by neuro-muscular electrical stimulation of the tongue muscle. It prevents tongue from rolling back.
Positional Therapy
In some cases where OSA is position-dependent, sleeping on side can significantly reduce apnea events by keeping the airway open. There are several types of positional therapies available over-the-counter in the market.
BongoRx
Bongo Rx is a small, simple medical device used to treat mild obstructive sleep apnea without a CPAP machine. It is non-motorized and consists of small valves inserted into the nostrils. These valves create resistance during exhalation to keep the airway open. It fits just inside the nostrils and uses your own breathing to create EPAP. When you breathe out, tiny valves close and push air back into your airway to help keep it open. It doesn’t need electricity, hoses, or batteries, and it’s portable, reusable, and FDA‑cleared with a prescription.
Medications
Zepbound (Tirzepatide): As of December 2024, this injectable medication is approved for adults with both sleep apnea and obesity. By mimicking a hormone called GLP-1, it induces weight loss leading to significant reduction in the severity of sleep apnea. It has side effects as well.
Inspire Hypoglossal Nerve Stimulator (HNS)
HNS is a treatment for sleep apnea that uses a small implantable device to keep the airway open. It has three parts: a stimulator in the chest, a lead on the hypoglossal nerve to move the tongue, and a sensor that detects breathing. When you inhale, the device sends mild pulses to push the tongue forward, stopping airway collapse. It turns off during exhalation and repeats each breath. Patients can control it with a remote, and it helps reduce apnea and improve sleep.
Lifestyle Changes That Can Help You Manage Sleep Apnea
While medical treatments are often necessary, lifestyle changes are a critical part of managing sleep apnea.
- Maintain a Healthy Weight: Losing weight can reduce the severity of symptoms by decreasing the fat stored around the neck.
- Review Medications: Be cautious with opioids, muscle relaxers, and certain anxiety medications, as they can slow breathing and relax airway muscles.
- Exercise Regularly: 30 minutes of moderate exercise can improve oxygen levels and sleep quality, even independent of weight loss.
- Adhere to Therapy: Consistency is key; using sleep apnea therapy regularly has been shown to reduce the chances of serious diseases associated with significant sleep apnea.
- Avoid Alcohol: Alcohol must be avoided because even in moderation, it significantly relaxes the throat muscles, leading to sleep apnea.